Clinical case: phage therapy of an infected diabetic foot
Doctors from the Giorgi Eliava Phage Therapy Center (Tbilisi, Georgia) published an article* describing four clinical cases of phage therapy for surgical wounds. We present one of them: the treatment of a diabetic foot infected with multidrug-resistant bacterial strains.
A 69-year-old man was admitted to the Phage Therapy Center in July 2017. He had type 2 diabetes, which had led to the development of an ulcer (diabetic foot syndrome) on his left foot several months prior to his presentation (Fig. 1). He had received several courses of antibiotic therapy, which were ineffective.
Laboratory findings : increased ESR (55 mm/h), increased HbA1c (7.6%), decreased INR (1.78), increased levels of creatinine (208.46 mmol/l) and uric acid (268.46 mmol/l).
X-ray of the foot showed changes typical of osteomyelitis.
Physical examination : ulcer about 5 cm in diameter with purulent exudate.
Microbiology : Analysis of the ulcer's bacterial colonization revealed the presence of strains of Staphylococcus aureus (the main causative agent), Burkholderia cepacia, and Enterococcus faecalis . All strains were multidrug-resistant.
Treatment
Among the ready-made bacteriophage preparations, staphylococcal bacteriophage and Intestifag were selected (contains bacteriophages specific against Shigella flexneri ( Serotypes 1,2,3,4 ) Shigella sonnei; Shigella newcastle; Salmonella paratyphi A, Salmonella paratyphi B; Salmonella typhimurium; Salmonella enteritidis; Salmonella choleraesuis; Salmonella oranienburg; E. coli; Proteus vulgaris; Staphylococcus aureus; P. aeruginosa; Enterococcus faecalis ). Bacteriophage against B. cepacia was absent.
Both phage preparations were administered orally, and Intestifag was also applied topically. Using a sterile syringe, 10 ml of Intestifag was applied to a gauze pad, which was then applied to the wound once daily. In addition, using a sterile catheter inserted into the wound, local irrigation with 2-3 ml of Intestifag was performed once daily for 7 days (Fig. 1b).
The patient received 20 ml of phage preparations orally (before taking the preparation, 100 ml of alkaline mineral water was used as an antacid). The course of treatment was 20 days, then after a 14-day break, the course was repeated. Additionally, the patient received Milgamma 100 mg of vitamin B complex and Actovegin 200 mg. The patient did not take antibiotics during treatment.
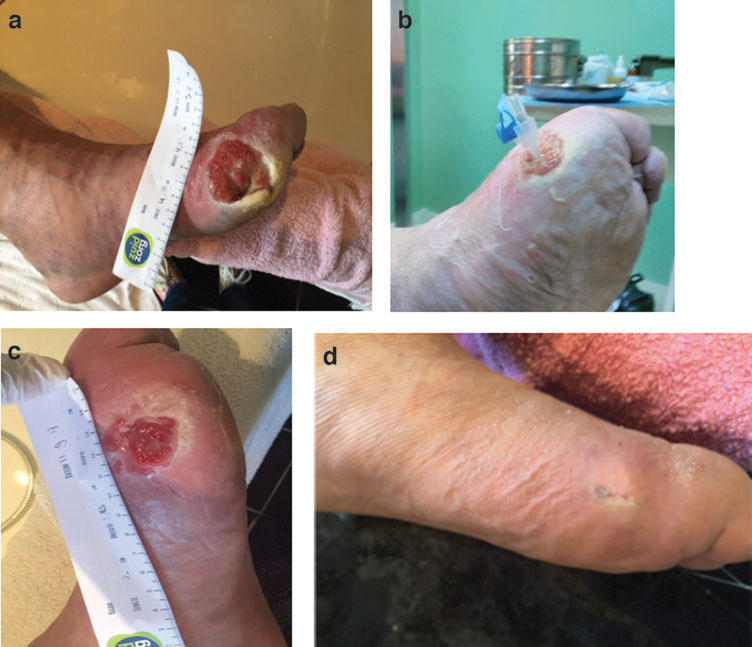
Fig. 1. Phage therapy of diabetic ulcer: (a) ulcer before the start of phage therapy; (b) catheter for introducing the phage preparation directly into the wound; (c) ulcer condition 6 weeks after the start of treatment; (d) complete wound healing; patient’s left foot after 1 year of observation (L. Nadareishvili et al., 2020).
Results
Five weeks after the start of treatment, the ulcer size had decreased to 2.4-2.5 cm, and by six weeks, to 2 cm (Fig. 1c). Wound healing and granulation tissue formation were visually observed. CT scans showed no signs of osteomyelitis.
No side effects of phage therapy were observed.
During 1 year of observation, no recurrences of diabetic foot infections were observed (photo after 12 months - Fig. 1d).
* Nadareishvili L., Hoyle N., Nakaidze N. et al. Bacteriophage Therapy as a Potential Management Option for Surgical Wound Infections. PHAGE: Therapy, Applications, and Research, 2020; 1 (3). DOI: 10.1089/phage.2020.0010

